The Menstrual Cycle
The Menstrual Cycle, Unboxed:
Getting Real About Menstrual Health
The menstrual cycle is a natural and powerful part of many people’s lives. It is your body’s way of preparing for the possibility of pregnancy, and it is nothing to be ashamed of.
Learning how it works helps you understand your health, your emotions, and your body better.

Not everyone who menstruates identifies as a woman. No matter your gender identity, you deserve care that respects and reflects who you are.
Phases of the Menstrual Cycle



Phases Broken Down




Disclaimer: Ovulation can be tricky to track—especially during early adolescence.
Periods often fluctuate due to stress, changes in routine, or natural hormonal shifts. Everyone’s cycle is different, and that is completely normal.
Want to learn more about ovulation? Click here
Understanding the Menstrual Cycle
The menstrual cycle is guided by several hormones that work together to prepare the body for a possible pregnancy. The three hormones shown in the graph are estrogen, progesterone, and luteinizing hormone (LH).
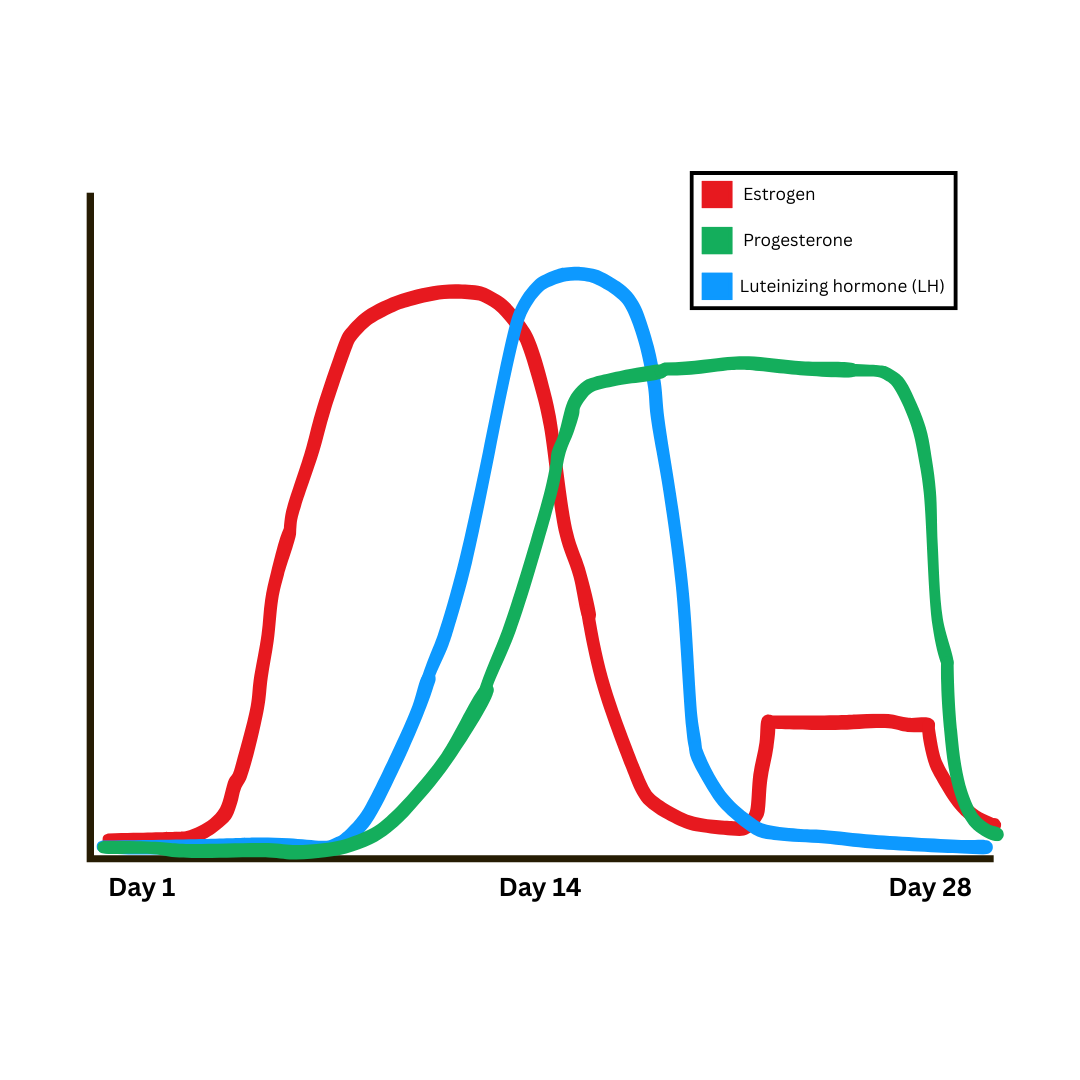
The first half of the cycle
At the start of the cycle, estrogen levels gradually increase as the ovaries begin developing follicles that contain eggs. Estrogen helps prepare the uterus by rebuilding the uterine lining after the previous period.
Ovulation
As estrogen continues to rise, it eventually reaches a level that signals the brain to release luteinizing hormone (LH). This sudden increase in LH is called the LH surge, and it triggers ovulation, which is when the ovary releases an egg.
After ovulation
Once ovulation occurs, the body begins producing more progesterone. Progesterone helps support and maintain the uterine lining in case a pregnancy occurs.
If pregnancy does not occur
If the egg is not fertilized, progesterone and estrogen levels drop. When these hormone levels fall, the uterine lining sheds. This shedding is what causes a menstrual period.
How Hormonal Birth Control Changes the Cycle
Many hormonal birth control methods contain synthetic estrogen and progestin (a hormone similar to progesterone). These hormones work together to prevent pregnancy in a few different ways.
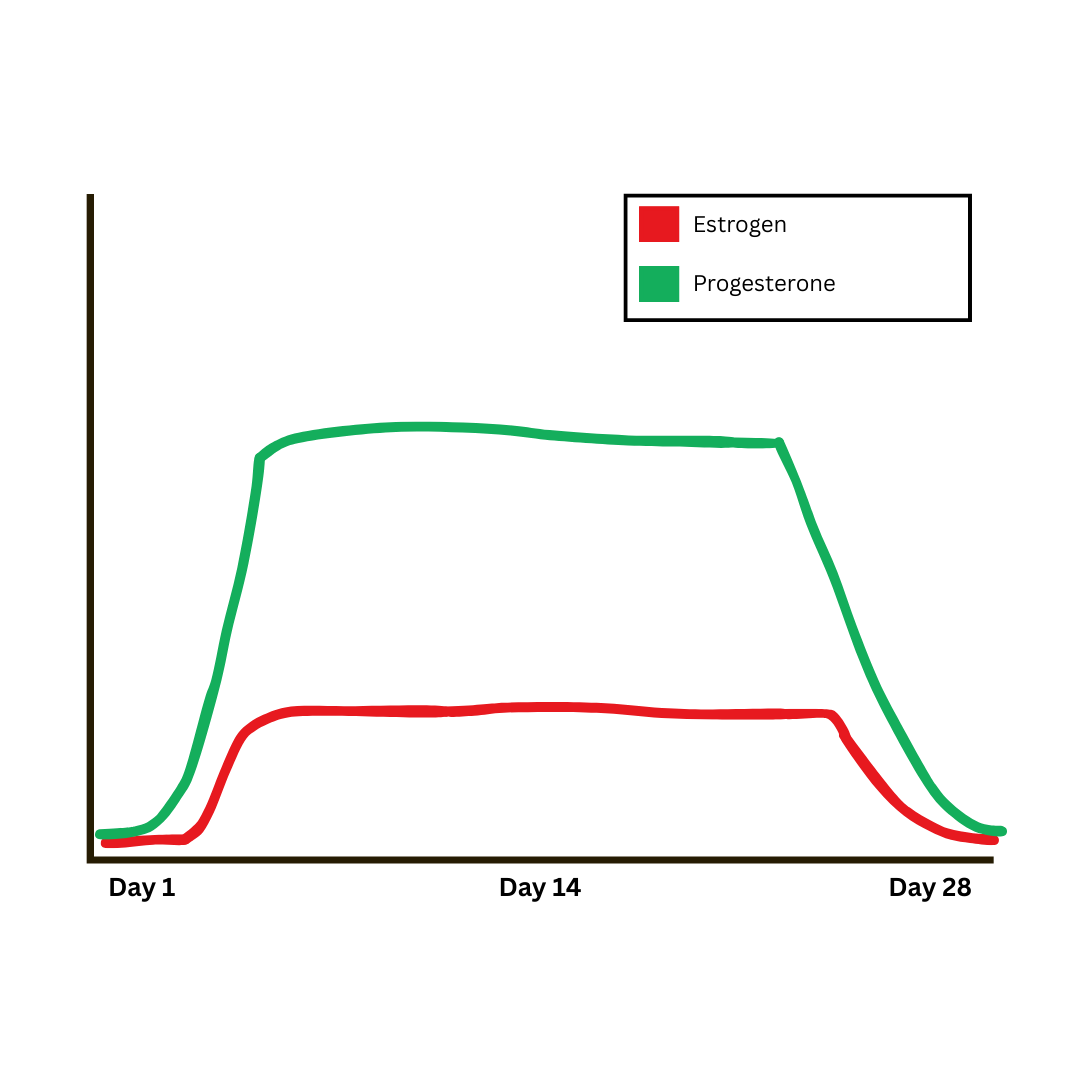
Preventing ovulation
Synthetic hormones keep estrogen and progestin levels steady, which prevents the normal hormone peaks seen in a natural cycle. This steady level signals the brain to suppress hormones like LH and FSH, preventing the LH surge that normally triggers ovulation.
Thickening cervical mucus
Progestin thickens cervical mucus, making it harder for sperm to travel through the cervix and reach an egg.
Changes to the uterine lining
Hormonal birth control can also thin the uterine lining, which makes it less likely that a fertilized egg could implant.
Why bleeding happens on birth control?
Many birth control pills follow a schedule of 21 active hormone pills and 7 placebo pills. During the placebo week, hormone levels temporarily drop. This drop can cause withdrawal bleeding.
This bleeding may look like a period, but it is not the same as a natural menstrual cycle.
When to pay attention to changes
Menstrual cycles can vary from person to person. Some fluctuation in timing or flow is normal. However, it may be helpful to speak with a healthcare provider if something feels unusual, such as:
Very heavy bleeding
Severe pain
Bleeding between periods
Missed periods when pregnancy is not possible
Your body’s cycle can change over time, and paying attention to those changes can help you understand what is normal for you.

What is Normal?
Everyone’s cycle is different and that is normal.
A typical menstrual cycle is 21 to 35 days long, and bleeding usually lasts 2 to 7 days. For some, periods are predictable. For others, they vary each month.
If something feels off, trust your instincts. you deserve to feel confident in your body.
Do not hesitate to talk to a healthcare provider or OB/GYN if you notice changes or have questions.
It is also common for periods to be irregular during adolescence, especially in the first few years after menstruation begins.
Irregular Periods
Irregular cycles might mean:
Skipping a period
Having periods too often or far apart
Heavier or lighter bleeding than usual


This can happen for many reasons, including:
Stress
Changes in weight or exercise
Birth control use
Health conditions like PCOS or thyroid issues
If your cycle is changing a lot or affecting your daily life, it is okay to talk to a healthcare provider. You are not being dramatic—it is your body, and you deserve answers.

When to Seek Help
It is always okay to ask questions about your cycle.
You might want to reach out to a provider if:
Period pain regularly interferes with your everyday life
Bleeding lasts over 7 days
No period for 3+ months
Bleeding between periods/after sex
Worried or confused about body

You deserve care that listens to your concerns and helps you feel more in control.
Which Menstrual Product Is Right for You?
There is no one-size-fits-all when it comes to period care. Whether you're new to menstruation or just looking to try something new, this guide can help you figure out which product might match your lifestyle, comfort, and needs.
Let’s break it down:
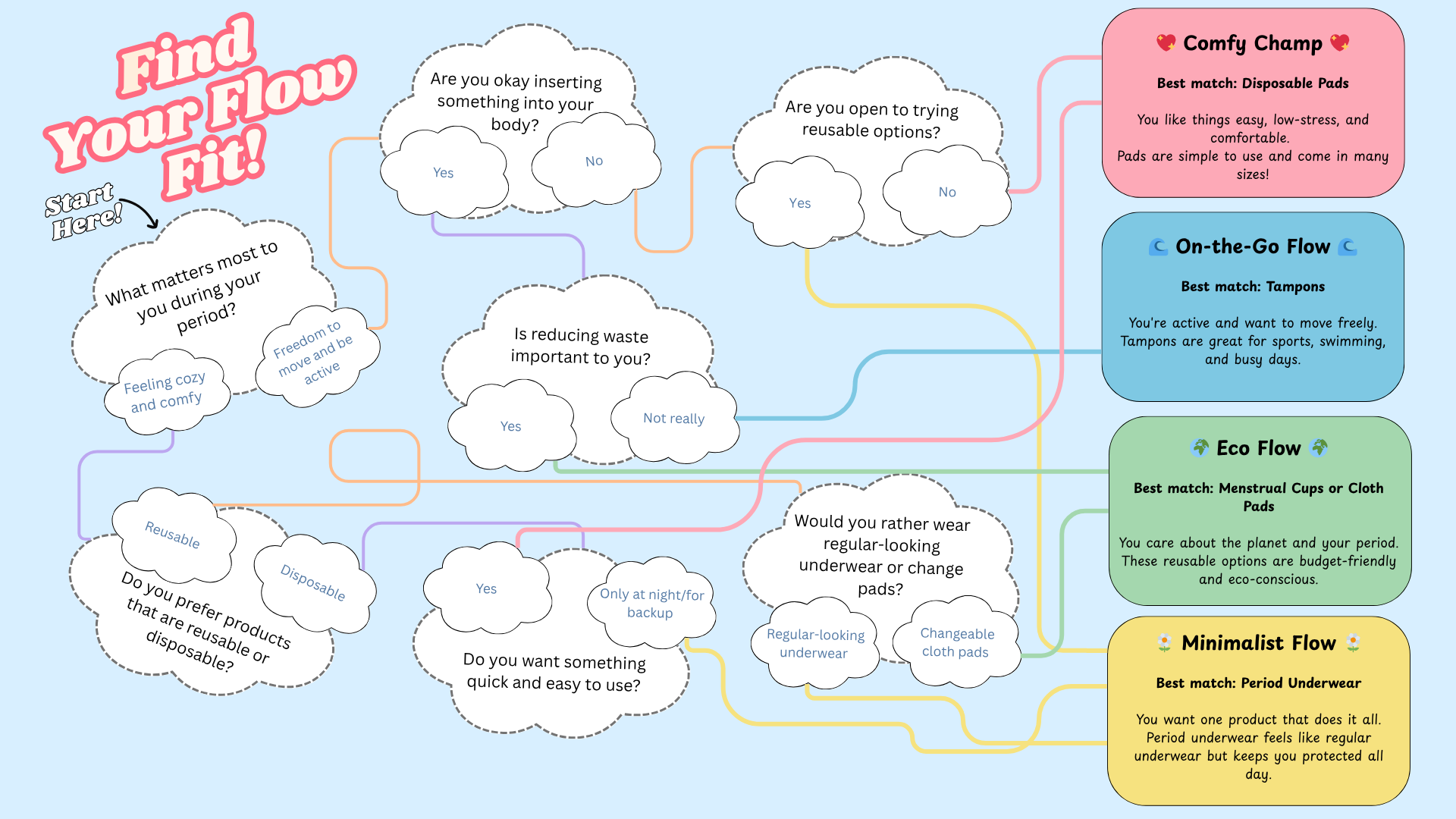
Find Your Flow Fit
Which period product fits your life best?
This little game is just for fun! It can help you explore different period products based on your comfort, lifestyle, and preferences. You do not have to use what your result says — but if it matches what you already use or want to try, that’s awesome!
Everyone's body and period experience is different, and there is no right or wrong way to manage your flow. Whether you are new to periods or just want to learn more, this can be a helpful place to start.
Now… let’s find your Flow Fit!
Birth Control and Your Period
Birth control can change your cycle, and that is expected!
Everyone’s body reacts differently, so your experience might not be the same as someone else’s. Some people have lighter periods, some stop getting them altogether, and some notice changes like spotting.
These changes are usually normal and nothing to worry about—but if something does not feel right, contact a medical provider you trust.

If you want to learn about different birth control methods, click here.
Here is a general idea of what you might notice with different methods:
The Pill, Patch, or Ring
These methods use hormones to prevent pregnancy.
You might:
Bleed less or skip your period (especially if you take it continuously)
Have more regular cycles
Notice spotting between cycles (especially at first)

The Shot (Depo-Provera)
A shot you get every 3 months.
You might:
Stop getting your period after a few months
Have irregular bleeding at first
Bleed more or less than usual
Hormonal IUD (like Mirena or Liletta)
Placed in the uterus and lasts several years.
You might:
Have lighter periods or no period at all over time
Spot irregularly at first
Feel cramping or notice changes as your body adjusts

Non-Hormonal IUD (Paragard)
This one has no hormones—just copper.
You might:
Still get your period monthly
Have heavier bleeding or more cramping at first
Adjust after a few months

The Implant (Nexplanon)
A small rod placed under your skin.
You might:
Bleed less, more, or not at all
Notice spotting, especially in the first 6–12 months
Have unpredictable periods